Hearing Loss and Dementia: What You Should Know
Learn how hearing loss changes the brain and can lead to isolation.
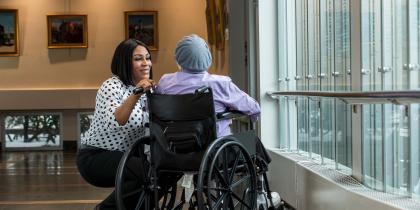
Hearing loss can mean more than just missing out on what people are saying. In fact, it can accelerate the onset of dementia. While that might strike you as an exaggerated statement, there is a high amount of medical research linking hearing loss to dementia. A study by Johns Hopkins University found that people with hearing loss were 24% more likely to experience cognitive decline compared to people with “normal” hearing.
Hearing loss can cause brain cells to decline or atrophy, contributing to the brain damage that results in dementia. At the Deanna and Sidney Wolk Center for Memory Health, where I work as a nurse practitioner, we take a comprehensive approach to diagnosing and treating dementia. Because we know hearing loss can contribute to dementia, it is one of the first things we assess a patient for.
But why does hearing loss accelerate cognitive decline?
Hearing and the brain
A healthy mind needs to stay active. Hearing loss dampens one of your major senses, restricting some of the stimulation the brain needs to thrive. The resulting stagnation will atrophy the cells responsible for processing audio signals.
Hearing loss can result in social isolation. You might shy away from interacting with people if you have trouble understanding what they’re saying. That isolation can exacerbate the lack of stimulation and lead to other health concerns as well.
Additionally, hearing loss shifts the structure of the brain and the connections created between nerve cells. Cells that originally processed sounds will shrivel or be reassigned to other functions. A study conducted by the Hearing Journal demonstrated a marked decline in brain tissue: participants with hearing issues lost more than a cubic centimeter of brain tissue each year compared with those without impaired hearing.
The loss of brain tissue essentially means less brainpower. As the areas used for speech and sound shrink, the brain has to work harder to collect information. This increased strain means that there is less energy for other parts of the brain — such as memory cells — to help process the information.
But the situation isn’t hopeless. There are ways to mitigate the effects of hearing loss!
Social isolation and depression can mimic dementia
There’s a complex interrelationship between hearing loss, social isolation, depression, and dementia.
The anxiety of not understanding what others are saying can lead to self-imposed isolation. Rather than struggling to have a conversation with other people, it may feel easier to avoid conversations altogether. Social isolation can be a risk factor for both depression and dementia. In fact, social isolation has been associated with about a 50% increased risk of dementia.
The negative effects on brain health caused by depression can mimic those of dementia. As such, distinguishing between depression and dementia can be a challenge since they exhibit some of the same symptoms: impaired concentration, apathy, and loss of appetite, among others.
Further complications arise from the fact that the cognitive struggles produced by hearing loss mimic the struggles of both depression and dementia. Comprehension difficulties are a byproduct of cognitive decline as well as hearing loss.
As a geriatric nurse practitioner, it is my job to help identify what is going on with a patient in order to connect them with the appropriate course of treatment.
Auditory testing: The first line of investigation
When patients come to me, they are being evaluated for their cognition and memory loss. Testing hearing is the first priority. Of course, I ask the patient directly about their hearing. However, self-diagnosing hearing loss can be a challenge.
Sometimes, my patients will report that they hear fine, but when I ask other family members, they say that they need to talk louder or that the TV is always very loud. That is an indication that there is some hearing loss, so it’s time for me to investigate further.
I might list out letters and ask them to tap when they hear the letter A. If they are tapping all the time or missing letters, that could be a sign of hearing loss. If a patient can’t hear a question I ask, they might guess at a response, resulting in something off-topic, or nod along to try to make it look like they understand. I can also have a patient try to repeat a word that was whispered in their ear.
A simple cause of hearing loss is the buildup of cerumen (earwax), so I use a scope to see in the ear canal. Once that is eliminated as a possibility, the next step is to refer the patient to one of the audiologists at the outpatient specialty clinic at Hebrew Rehabilitation Center to make sure that there isn’t any loss of hearing function. If there is, then the next step might be hearing aids.
Common objections to wearing hearing aids
This is where there can be some resistance. In fact, many adults wait over 10 years to get hearing aids. While there are valid concerns around getting hearing aids, an audiologist can help you come up with a solution that meets your needs.
It is important to find a solution because of the crucial role hearing can play in combating dementia. Hearing aids have been shown to reduce the risk of dementia by 18%. It is also believed that addressing hearing loss reactivates the nerve cells responsible for auditory processing and could recover some of what was lost.
Some people are self-conscious about wearing hearing aids because they’re worried it means “looking old.” Remember that hearing aids aren’t exclusively worn by older people! They’re for anyone experiencing hearing loss, which affects people of all ages.
Hearing aids can also be forgotten, lost, run out of batteries, or be uncomfortable to adjust to. If you’re concerned about the appearance or physical sensation of wearing a hearing device, know that they are getting smaller and less noticeable.
Another common concern is that hearing aids are usually not covered by insurance. Some plans offer optional coverage for hearing aids, but those options are not widely available. Fortunately, they are becoming cheaper, with over-the-counter devices available. Finding a hearing aid that works for your preferences and budget can make a big difference in making you feel more comfortable.
Supporting someone experiencing hearing loss
One of the most effective techniques for helping my patients feel more willing to explore the use of hearing aids is encouragement from their family. As a family member, you can emphasize that you are coming from a place of love and support.
You can gently remind your loved one how improved hearing would enhance shared experiences for the whole family. Improved hearing will allow them to more actively participate in their own life, whether that means listening to cheering crowds at an event, engaging in dinner conversations, or hearing the laughter of their grandchildren.
With education and support, many people will find that hearing aids can be a useful tool for staying engaged in the relationships and activities that give their lives meaning. Of course, remember that your loved one cannot be forced into using hearing aids, regardless of what you think is best for them.
Diagnosing dementia
Once we’ve ruled out hearing as the issue, we can move on to different diagnostic testing to assess whether a patient has dementia and, if so, the exact cause. This can include neuropsychological evaluation, brain MRI, amyloid PET scan, DAT scan, and biomarker confirmation for Alzheimer’s disease with lumbar puncture.
Early signs of dementia, such as memory loss that disrupts daily life, can be cause for concern. That said, cognitive decline and memory loss don’t automatically mean you have dementia. Other conditions that mimic cognitive impairment include reversible causes such as thyroid disease, vitamin deficiencies, drug reactions, mental health conditions, and alcohol abuse. It is important to see a doctor to obtain an accurate diagnosis and establish a treatment plan that works for you.
Outpatient memory care at Hebrew SeniorLife
If you’re concerned about memory loss, the Wolk Center for Memory Health at Hebrew SeniorLife can help you identify the cause, whether it’s hearing loss or something more complicated. The earlier you seek care, the more options you have for treatment and lifestyle interventions.
If a diagnosis is made, we can also work with you and your family to create a treatment plan based on your own individual needs and goals. Call us at 617-363-8600 or contact us online today.
Blog Topics
Learn More
Free Guide to Brain Health
Download our free guide, “Optimizing Your Brain Health,” for expert advice on boosting brain health at any age. Explore practical tips and resources from Hebrew SeniorLife’s Deanna and Sidney Wolk Center for Memory Health.

Wolk Center for Memory Health
The Deanna and Sidney Wolk Center for Memory Health at Hebrew SeniorLife provides outpatient memory care services, in person and virtually, for people living with cognitive symptoms — and for their families and caregivers.
Coping with Memory Loss
From our Wolk Center for Memory Health to our Adult Day Health program to Assisted Living to Memory Care Assisted Living, we offer a wide range of memory care services and support.




