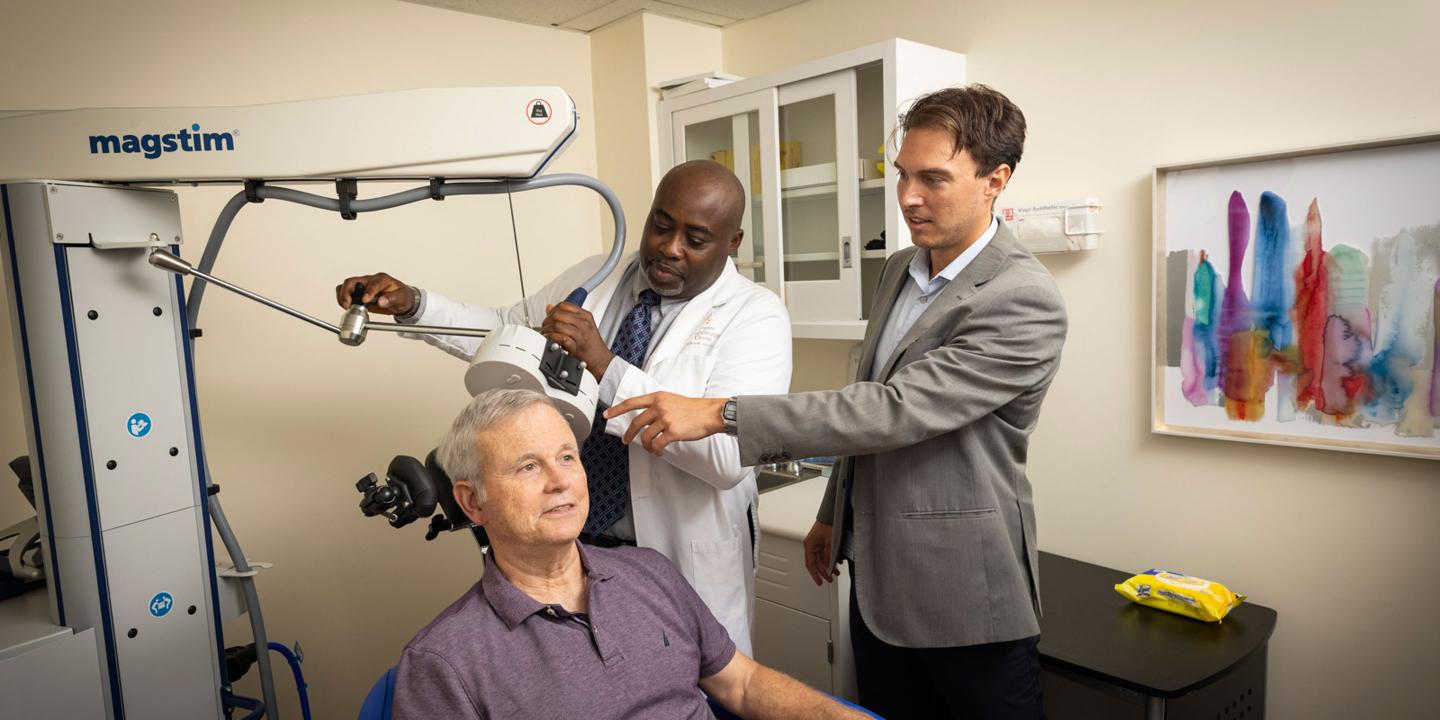
Modern treatment for depression, personalized for you
Depression is common in older adults, but it’s not a normal part of growing older. Depression is a treatable medical condition that’s more common in seniors with dementia or chronic health conditions.
Treating depression in older adults can be more complicated than in younger people, in part because medications for depression can interact with other treatments, and medications are both less effective and more likely to cause side effects in older adults.
New approaches to treating geriatric depression are desperately needed. That’s why the Deanna and Sidney Wolk Center for Memory Health offers Transcranial Magnetic Stimulation (TMS).
The Wolk Center for Memory Health offers the only TMS program in New England that specializes in treating geriatric depression. It’s offered under the expert oversight of Medical Director and cognitive neurologist Dr. Alvaro Pascual-Leone, a pioneer in the use of non-invasive brain stimulation.
What is Transcranial Magnetic Stimulation (TMS) therapy?
Transcranial Magnetic Stimulation is a non-invasive, personally-tailored approach to treating depression. TMS modulates networks in the brain that are responsible for mood regulation.
TMS is highly safe and effective at treating medication-resistant depression - about 60% of patients experience an improvement in symptoms, and lasting side effects or complications are very rare. By contrast, patients who haven’t responded to at least one medication for depression have only a 3% chance of responding to any other medication.
At the Wolk Center for Memory Health, we use the latest generation of FDA-approved TMS equipment. Our staff and technicians strictly adhere to all training and treatment guidelines endorsed by the International Federation for Clinical Neurophysiology.
You’ll be awake and aware during the treatment, which generally causes little discomfort - just a tapping sensation on your head and the clicking sound of the stimulation, which will be muffled by earplugs provided to you. Treatment sessions last approximately 45 minutes, and you’ll be asked to come five days a week for about four weeks.
Throughout the treatment process, you’ll be carefully monitored by our psychiatrist. TMS is covered by most private insurance and Medicare.
Who qualifies for TMS?
At the Wolk Center, we specialize in treating older adults, but we welcome people of all ages.
TMS is approved for treatment-resistant depression, which means, for example, that you’ve tried at least two antidepressant medications and experienced no relief or had to discontinue them because of side effects. The treatment is appropriate for people experiencing dementia or cognitive decline as well as depression, and can improve cognition in addition to alleviating the symptoms of depression.
TMS is also approved for anxiety disorders, which are common in older adults, are often unrecognized and undertreated, and represent a major cause of disability. TMS can be very helpful for patients with anxiety disorders and can substantially improve well-being and quality of life.
You’ll need a referral from your psychiatrist to begin treatment, and we’ll keep them and your primary care physician updated on the progress of your care.
Interested in learning more about TMS therapy at the Wolk Center for Memory Health?
Contact Us
After TMS, it felt like someone scraped all the despair, heaviness, and depression from my body. I felt and feel so much lighter and better. People tell me that I smile a lot more than I used to.”
John Bengel, 78. Read John's story.
Frequently Asked Questions
Read more to learn about TMS, the Wolk Center for Memory Health, and what you can expect.
During your first visit, you’ll meet with our psychiatrist, who will go over your medical and depression history, explain the treatment process, and answer any questions you may have.
At your second visit, you’ll meet with the technician to map your brain and establish the right location and intensity for the treatment. The mapping process is painless. You’ll sit in a chair wearing an adhesive tracker on your forehead. A camera establishes the location of the part of your brain that will be targeted for the treatment.
Following the mapping you’ll receive your first TMS treatment. You’ll sit in a comfortable chair while we place an electromagnetic coil next to your head. We’ll personalize the intensity of the stimulation, then record it for future visits.
During subsequent visits, you’ll go directly to the technician for treatment. Once a week you’ll meet with our psychiatrist to review your progress. Of course, the entire team is always available should you have any questions.
The treatment session itself lasts about 45 minutes and is almost pain-free. We’ll place an electromagnetic coil next to your head while you sit comfortably in a chair. Some people describe what they feel during treatment as a tapping or vibrating sensation on their head.
You may experience twitching and/or blinking, because the treatment stimulates parts of your brain that control movement in your hands and feet. This is completely normal, and only lasts during the treatment itself. We’ll carefully calibrate the intensity of the treatment to minimize this effect.
The machine itself makes a loud clicking noise (similar to an MRI machine), so we’ll give you ear plugs to wear during treatment. Of course, the technician will be with you at all times during the treatment session.
After each treatment session is over, you can return to your normal activities immediately.
Most patients come for treatment five days per week for about four to six weeks, following by four to six additional tapering sessions over a span of two weeks. When symptoms are improved, relief can last for up to a year. If symptoms of depression return, you can complete another course of treatment.
TMS is highly safe and effective at treating treatment-resistant depression - about 60% of patients experience an improvement in symptoms, and lasting side effects or complications are very rare. By contrast, patients who haven’t responded to at least one medication for depression have only a 3% chance of responding to any other medication.
TMS is an outpatient treatment, and patients can return to their normal activities immediately.
There are very few side effects from TMS, and if they do occur they tend to be mild, improve shortly after an individual session, and decrease over time with additional sessions. Side effects may include:
- Headache
- Scalp discomfort at the site of stimulation
- Tingling sensation or twitching of facial muscles during the treatment session
- Lightheadedness
We’ll adjust the intensity of your treatment to minimize any possible discomfort or side effects.
You may begin experiencing relief from your symptoms in as little as two weeks after beginning treatment. When the treatment is effective, TMS can bring relief for up to a year. If your symptoms return, you can choose to undergo another round of treatment. Research shows that patients who respond to a first course of treatment continue to show positive response to subsequent treatments, should those be necessary.
Yes, TMS can be used in conjunction with medication and/or therapy.
TMS treatment at the Wolk Center for Memory Health is overseen by an expert and accomplished care team.
- The Wolk Center’s Medical Director, cognitive neurologist Dr. Alvaro Pascual-Leone, provides oversight for all patient care. Dr. Pascual-Leone is also senior scientist at Hebrew SeniorLife’s Hinda and Arthur Marcus Institute for Aging Research, and a professor of neurology at Harvard Medical School. He is a pioneer in the use of non-invasive brain stimulation.
- At your first meeting and once a week thereafter, you’ll meet with our psychiatrist to discuss your medical condition and your care. The psychiatrist also oversees the treatment and ensures a high quality of care for all patients.
- Our neuropsychologist ensures the quality of care for our patients, provides overall oversight of the TMS program, supervises the technician’s work, guarantees quality control procedures are in place, and keeps the program up-to-date with the latest best practices.
- A fully-trained technician will provide the TMS treatment, ensure your comfort, monitor you for side effects during treatment, and make adjustments as necessary.
TMS is different from Electroconvulsive Therapy (ECT), commonly known as “shock therapy.” Both use electricity, but the mechanism and experience are very different.
TMS is an outpatient non-invasive treatment that selectively modifies activity in specific areas of the brain. TMS does not require anesthesia. During treatment, patients are awake and alert, and can immediately return to their normal activities. TMS uses electromagnetic induction to introduce current in the brain and does not apply current directly to the scalp. It is not painful and generally has only mild side effects.
By contrast, ECT works by applying direct electric currents to the patient's head while they are sedated, intentionally causing a "therapeutic seizure" in order to reset the brain.
Both treatments can be extremely effective in alleviating the symptoms of depression, but TMS has similar efficacy with fewer risks and much less potential for side effects.
TMS is covered by most private insurance and Medicare. Check with your insurer for specific coverage.
Yes, you need a referral from your treating psychiatrist. We’ll keep in communication with them and any other members of your care team that are necessary, such as your PCP.
The Deanna and Sidney Wolk Center for Memory Health at Hebrew SeniorLife is located at 1200 Centre Street on the campus of Hebrew Rehabilitation Center in Boston. We are conveniently located at the intersection of Centre Street and the VFW Parkway near the Roslindale, Jamaica Plain, and West Roxbury neighborhoods. We are wheelchair-accessible and there is an MBTA bus stop in front of the building.
Use the lower B1 entrance on Centre Street for the easiest access to the Wolk Center for Memory Health. Hebrew Rehabilitation Center front desk staff will be happy to direct you down a short hallway to our office.
Yes, there is free valet parking at our lower B1 entrance on Walter Street.